Abdominal Aortic Aneurysm (AAA)
What is an abdominal aortic aneurysm?
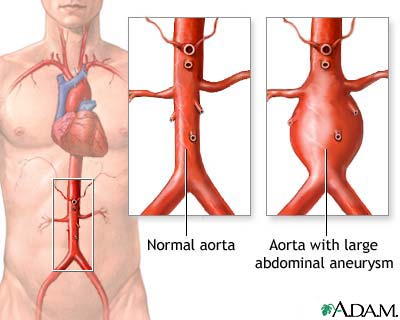
An AAA occurs when the aorta, the large blood vessel that supplies blood to the abdomen, pelvis, and legs, becomes abnormally large and balloons outward. An aneurysm can occur in any part of the aorta and can happen to other vessels, but the most common aneurysm occurs in the abdominal aorta (Figure 1).
An AAA occurs when the aorta, the large blood vessel that supplies blood to the abdomen, pelvis, and legs, becomes abnormally large and balloons outward. An aneurysm can occur in any part of the aorta and can happen to other vessels, but the most common aneurysm occurs in the abdominal aorta (Figure 1).
Who is at risk for a AAA?
The risk factors for developing an AAA include COPD, genetic factors, hypertension, hyperlipidemia, being male, obesity, and a history of smoking. While a AAA can happen to anyone, the condition is most commonly observed in males over 60 who have one or more risk factors.
The risk factors for developing an AAA include COPD, genetic factors, hypertension, hyperlipidemia, being male, obesity, and a history of smoking. While a AAA can happen to anyone, the condition is most commonly observed in males over 60 who have one or more risk factors.
What are the signs/symptoms of a AAA?
Aneurysms themselves usually develop slowly over many years and are asymptomatic unless the aneurysm expands rapidly, ruptures, or a dissection occurs. The symptoms of an AAA are mild and often go undetected. These symptoms include back pain, the feeling of fullness between meals, nausea at night, abdominal pulsation, weak peripheral pulses, and a difference in blood pressure between the right and left arm. In the event of a rupture, an individual may experience severe, sudden pain in the abdomen or back that radiates to the groin, buttocks, or legs, diaphoresis, dizziness, nausea/vomiting, tachycardia, or shock.
Aneurysms themselves usually develop slowly over many years and are asymptomatic unless the aneurysm expands rapidly, ruptures, or a dissection occurs. The symptoms of an AAA are mild and often go undetected. These symptoms include back pain, the feeling of fullness between meals, nausea at night, abdominal pulsation, weak peripheral pulses, and a difference in blood pressure between the right and left arm. In the event of a rupture, an individual may experience severe, sudden pain in the abdomen or back that radiates to the groin, buttocks, or legs, diaphoresis, dizziness, nausea/vomiting, tachycardia, or shock.
How is a AAA diagnosed and how is it treated?
Aneurysms are typically detected by chance during radiology studies for other conditions because the symptoms aren’t always obvious. A physical examination with palpation of the abdomen may reveal a lump in the abdomen, a pulsatile mass, or a rigid abdomen. The presence of an AAA can be confirmed by an angiogram, CT of the abdomen, or an abdominal ultrasound.
The treatment of the AAA depends on the severity of the condition. If the aneurysm is small, surgery is rarely performed, and screening will be performed every 6 months to monitor the size of the AAA. If the aneurysm is larger than 5.5 cm and is expanding rapidly, there are two surgical options:
Aneurysms are typically detected by chance during radiology studies for other conditions because the symptoms aren’t always obvious. A physical examination with palpation of the abdomen may reveal a lump in the abdomen, a pulsatile mass, or a rigid abdomen. The presence of an AAA can be confirmed by an angiogram, CT of the abdomen, or an abdominal ultrasound.
The treatment of the AAA depends on the severity of the condition. If the aneurysm is small, surgery is rarely performed, and screening will be performed every 6 months to monitor the size of the AAA. If the aneurysm is larger than 5.5 cm and is expanding rapidly, there are two surgical options:
- A traditional open repair- a large abdominal incision is made and the abnormal vessel is replaced with a graft of man made material (Figure 2).
-
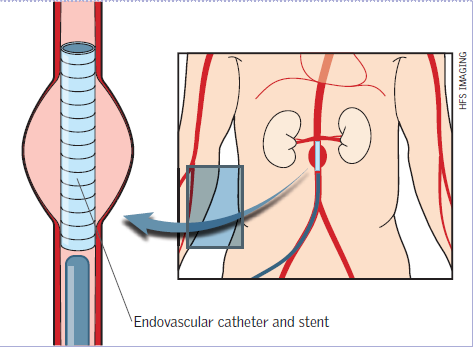
Endovascular stent grafting- a small surgical incision is made near the groin and a stent is inserted into the femoral artery along with a synthetic graft. Using x-ray imaging, the doctor guides the stent up to the aorta and attaches it to the walls of the aorta. Eventually, the aneurysm will shrink around the stent (Figure 3).
Why is an AAA a life threatening condition?
An aneurysm is benign until it gets too big and either causes a rupture or a dissection. When the AAA begins to tear or rupture, it is a true medical emergency. Less than 80% of patients survive a ruptured AAA.
An aneurysm is benign until it gets too big and either causes a rupture or a dissection. When the AAA begins to tear or rupture, it is a true medical emergency. Less than 80% of patients survive a ruptured AAA.
Sources
Bhimji, S. (2012). Abdominal aortic aneurysm. In A.D.A.M. Medical Encyclopedia. Retrieved March 28, 2014 from
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001215/
Kimura, T., Yoshimura, K., Aoki, H., Imanaka-Yoshida, K., Yoshida, T., Ikeda, Y., & ... Matsuzaki, M. (2011). Tenascin-C is
expressed in abdominal aortic aneurysm tissue with an active degradation process. Pathology International, 61(10),
559-564. doi:10.1111/j.1440-1827.2011.02699.x
Lederle, F. (2009). In the clinic. Abdominal aortic aneurysm. Annals Of Internal Medicine, 150(9), ITC5-1-15; quiz ITC5-16.
doi:10.7326/0003-4819-150-9-200905050-01005
Bhimji, S. (2012). Abdominal aortic aneurysm. In A.D.A.M. Medical Encyclopedia. Retrieved March 28, 2014 from
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001215/
Kimura, T., Yoshimura, K., Aoki, H., Imanaka-Yoshida, K., Yoshida, T., Ikeda, Y., & ... Matsuzaki, M. (2011). Tenascin-C is
expressed in abdominal aortic aneurysm tissue with an active degradation process. Pathology International, 61(10),
559-564. doi:10.1111/j.1440-1827.2011.02699.x
Lederle, F. (2009). In the clinic. Abdominal aortic aneurysm. Annals Of Internal Medicine, 150(9), ITC5-1-15; quiz ITC5-16.
doi:10.7326/0003-4819-150-9-200905050-01005